Cervical Stenosis, Myelopathy and Radiculopathy
General Information
The cervical spine refers to that portion of the spinal column that is within our neck. This portion of the spine needs to be flexible enough to allow us to turn our head from side to side and up and down, but at the same time needs be strong enough to protect the delicate spinal cord and spinal nerves that travel through it.
he spinal cord is like the main cable that brings television signals to the house. The spinal nerve roots are branches of the main cable that carry signals to each room within a house. The spinal cord carries signals from the brain into our arms, legs and body and, at the same time, carries signals back to the brain from our arms, legs and body. The spinal nerve roots control individual muscles or are responsible for feeling in certain parts of the arm or leg.
Cervical myelopathy refers to a loss of function in the upper and lower extremities secondary to compression of the spinal cord within the neck. Cervical radiculopathy refers to a loss of function in a specific region within the upper extremity secondary to irritation and / or compression of a spinal nerve root in the neck.
Image: X-ray of neck, showing degenerative spurs between C5 and C6
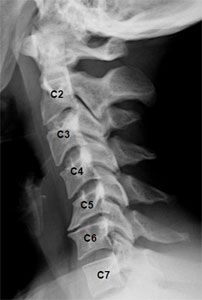
What are the symptoms?
Cervical myelopathy tends to creep up on patients in most cases. It can result in subtle changes in the way their hands work. Patients feel their hands are clumsier; they may drop objects more often, they may not be able to button their shirts as easily as they could, or their handwriting may become worse. Patients may develop unsteadiness, requiring holding onto objects more frequently while walking. Their gait may become noticeably wobbly. At times, they feel their brain doesn’t know exactly where their legs are in time and space. In extreme cases, patients may develop more profound weakness and numbness in their arms and legs and rarely changes in bowel or bladder control.
Cervical radiculopathy will manifest itself as pain traveling from the neck into a specific region of either arm, forearm or hand. In many instances, this will be accompanied by numbness in a similar distribution or weakness in specific muscles in either the arm, forearm or hand.
What is the natural history of these conditions
(What could I expect if I do nothing?)
The “natural history” of cervical radiculopathy depends in large part on how long the patient has had symptoms for. In patients who present with very early symptoms, the prognosis is generally very good. Most of these patients will have complete resolution of their pain, numbness and weakness over a 6-12 week period.
In patients who have had symptoms for a slightly longer period of time, the prognosis is less clear. Some patients will go onto complete resolution of pain with (and, in some cases, without) limited treatment such as modification of activities, heat, ice, physical therapy or over-the-counter medications. Approximately one third of these patients will have some lingering degree of symptoms that they may be able to cope with. A small percentage will have symptoms that are unbearable and may need further treatment.
The “natural history” of clinically obvious cervical myelopathy is somewhat more guarded. The consensus is that patients with myelopathy will have progression of symptoms. What is not known is when the symptoms will progress, how much they will progress or how rapidly they will progress. Approximately 75% of patients will have stepwise deterioration in their function with stable periods in between the episodes of deterioration. Twenty percent will have slow steady deterioration and another 5% will have rapid deterioration.
How is it diagnosed?
You should see your NASS doctor if you have worsening function in your arms and/or legs and if your primary care physician feels that this is related to your cervical spine. If you have persistent pain, numbness or weakness in one of your arms that is not relieved following a short period of observation, you should certainly see your NASS doctor.
Your NASS doctor will begin by letting you relate the history of how your symptoms began and how they progressed. You will be asked a series of questions and a physical examination then carried out that is directed primarily at your neck, and nerve function in your arms and legs. Your NASS doctor will check your balance, test your gait.
X-rays may be requested and will in some patients show signs of degenerative changes in the disc spaces or facet joints. Bending x-rays of the neck may show a small degree of “slip slide” between the neck vertebrae.
Magnetic resolution imaging [MRI] of the neck may be ordered. MRI pictures allow your NASS doctor to visualize structures that may be impinging on the spinal cord or the nerve branches. In some patients, injection of dye into the spinal cord [myelogram] may be required and this is followed by CT scans [computerized tomography].
Electrical testing of the nerves and spinal cord is requested in some patients. Electromyogram [EMG] and nerve conduction studies help distinguish cervical radiculopathy from other nerve problems in the arm and forearm such as carpal tunnel syndrome. Somatic sensory evoke potentials [SSEP] are electrical tests that study signal conduction through the spinal cord and may be ordered in some patients with cervical myelopathy.
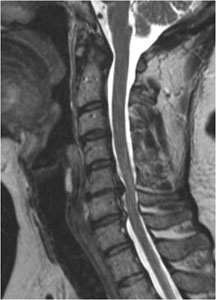
Image: MRI of neck, showing degenerative changes and severe spinal cord compression at C5/C6 and C6/C7
What treatments are available?
Most patients with cervical radiculopathy will be treated initially with non-operative measures. These measures typically include a short period of modification of activities. Modification of activities may include simple techniques such as changing the height of your computer monitor or the height of your chair at work. Your doctor may recommend applying ice or head to the painful area, or using over-the-counter anti-inflammatory medications judiciously, keeping in mind that overuse of any medication can be accompanied by unwanted side effects. Prolonged bed rest can lead to deconditioning and is generally not recommended.
In patients whose pain is not controlled with these measures, stronger medications such as prescription anti-inflammatory agents, muscle relaxants or narcotic analgesics may be required for a short period of time. Physical therapy is an important part of the rehabilitation process. Your physical therapist will carry out an evaluation of your function, and then instruct you on proper ergonomics and a gentle program of stretching and flexibility. As the pain resolves, mild strengthening exercises will be instituted. A primary benefit of physical therapy conditioning is avoidance of secondary stiffness or inflammation at your shoulder, elbow or elsewhere in the neck and upper extremities, commonly seen in patients who have pain and weakness.
In some patients with cervical radiculopathy, your NASS doctor may recommend injection treatments for your problem. Most commonly, these will be epidural steroid injections. These are targeted injections of corticosteroid into the area around the nerve that is inflamed in your neck. The purpose of the injection is to reduce the inflammation and relieve the pain associated with the irritated nerve.
In patients with mild cervical stenosis and without clinically obvious myelopathy, cautious nonoperative care is an option. This generally begins with a thorough education regarding their condition. Patients need to understand that narrowed dimensions of their spinal cord can predispose them to myelopathy at some point in the future.
Patients should be cautious to avoid situations or injury that might place their spinal cord at more risk. A short period of immobilization in a soft cervical collar may be helpful in some patients. Physical therapists can help with instructions on proper gait mechanics and the use of canes or walkers that can prevent falls. Occupational therapists can provide suggestions that help with everyday tasks such as bathing, dressing, opening jars or turning keys.
In patients who have narrowing of the space for the spinal cord, progressive myelopathy may be precipitated by the development of degenerative changes with age, injury to the already compressed spinal cord from a fall or motor vehicle collision, spinal instability or a combination of all of the above. If symptoms of cervical myelopathy are evident or progressing, you ought to be assessed by your NASS doctor.
Surgery for Cervical Stenosis, Myelopathy and Radiculopathy
In those patients where nonoperative measures are unsuccessful, surgical measures provide a good option. Your NASS doctor may recommend surgical intervention for cervical radiculopathy either through the front [anterior] or the back [posterior] of the neck, or both the front and back of your neck. Several factors will be considered by your NASS doctor in choosing the type of surgery you undergo. These will include the exact location of any compression on your spinal cord or nerve branches, the number of levels at which there is compression, the overall alignment of your cervical spine and your overall medical condition.
When surgery is carried out through the front of the neck, a small incision is made in the front of your neck. The tissues are gently moved to the side and the cervical vertebrae easily accessed. The structures impinging on the nerve root are removed. Frequently a block of bone obtained from a bone bank or your pelvis will be inserted in the disc space and a metal plate and screws will be used to stabilize two vertebra. Anterior surgery may be required at more than one level and may require removal of the discs and the vertebrae. Following surgery you may be in a neck brace for a short period of time depending on the surgical procedure.
When surgery is carried out through the back [posterior] of the neck, a small incision is made directly over the area where the nerve branches off of the spinal cord. A high speed burr may be used to remove some of the bone spurs impinging on the nerve branch. Small disc fragments can be removed through this hole. Following surgery, a period of immobilization may be used.
Posterior surgery can also involve a wider decompression of the entire cervical spinal cord through two operations: laminectomy and laminoplasty. In both of these operations, the pressure on the spinal cord is relieved by removing portions of the back of the vertebra. In laminectomy, the back of the vertebra is completely removed. In laminoplasty, a hinge is created on one side of the back of the vertebra and the lamina lifted up on this hinge to make room for the spinal cord. Occasionally metal screws and plates are used following either of these operations to stabilize the cervical spinal column.
